#COVID-19: Comparing provinces with other countries 12 January Update
2022/01/13 Leave a comment
Steep rise of infections remains the main story, along with resulting increases in hospitalizations and ICUs.
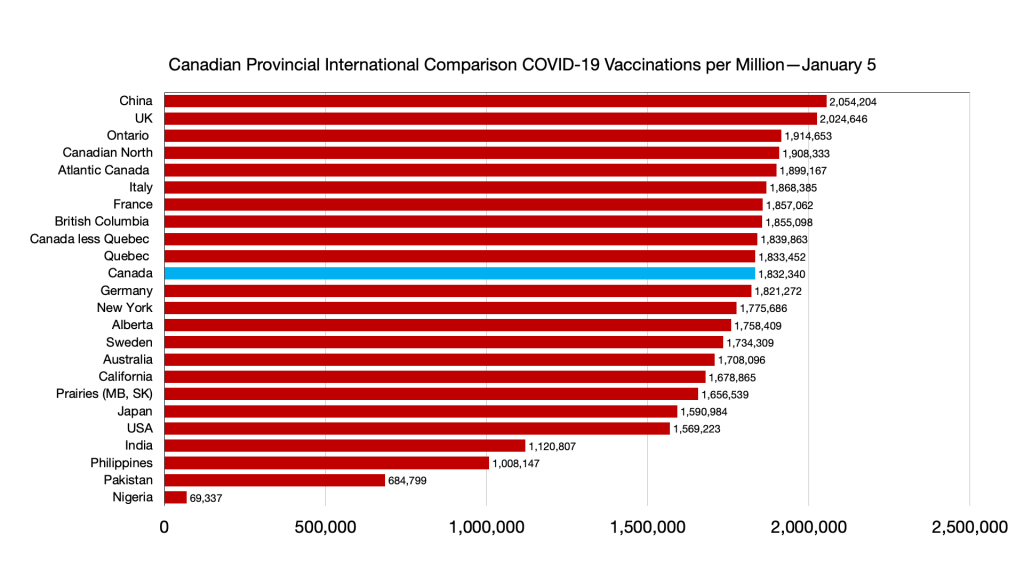
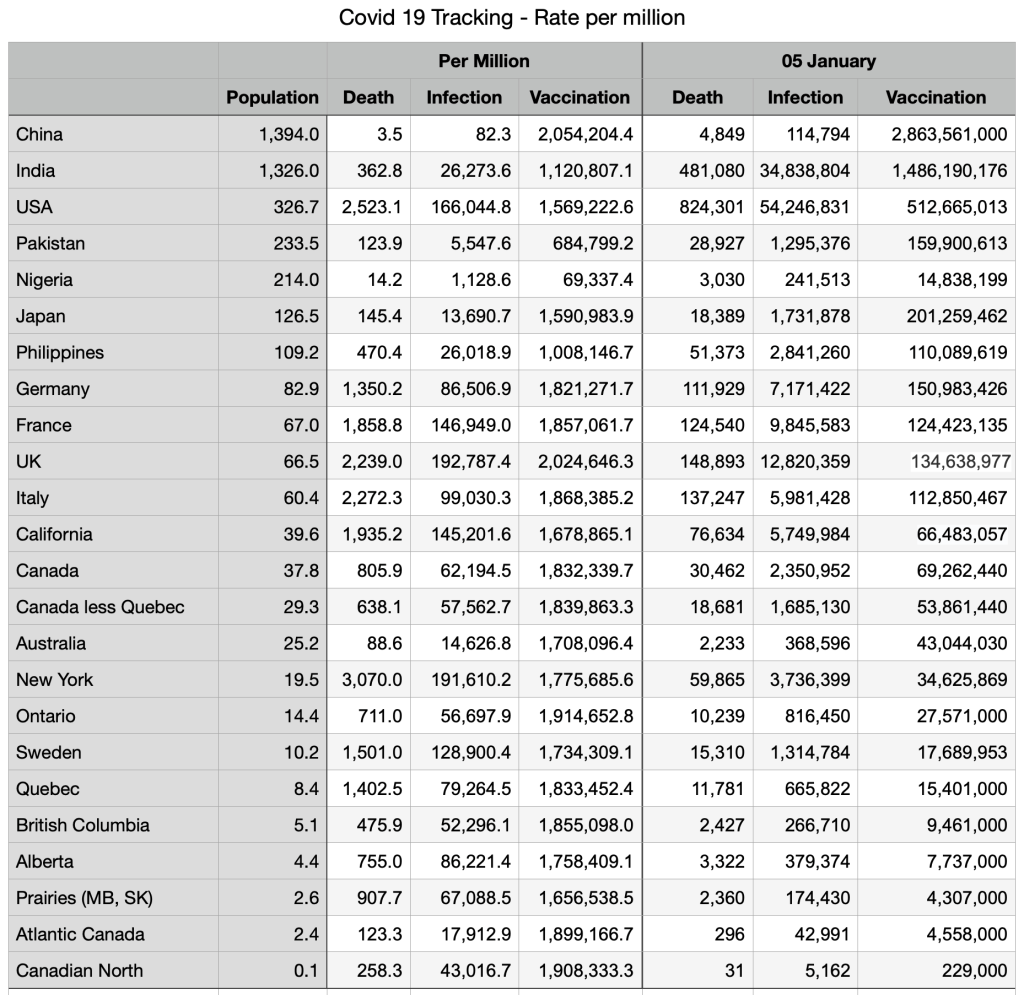
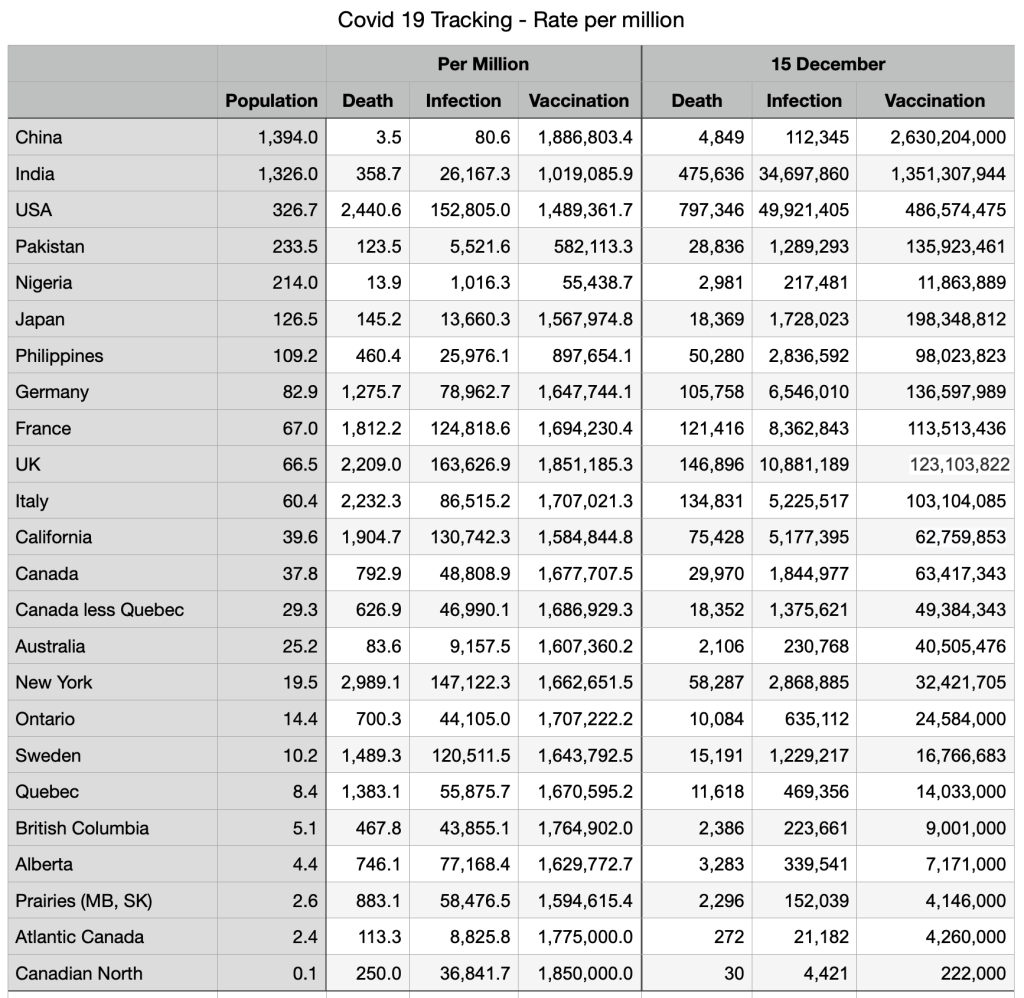
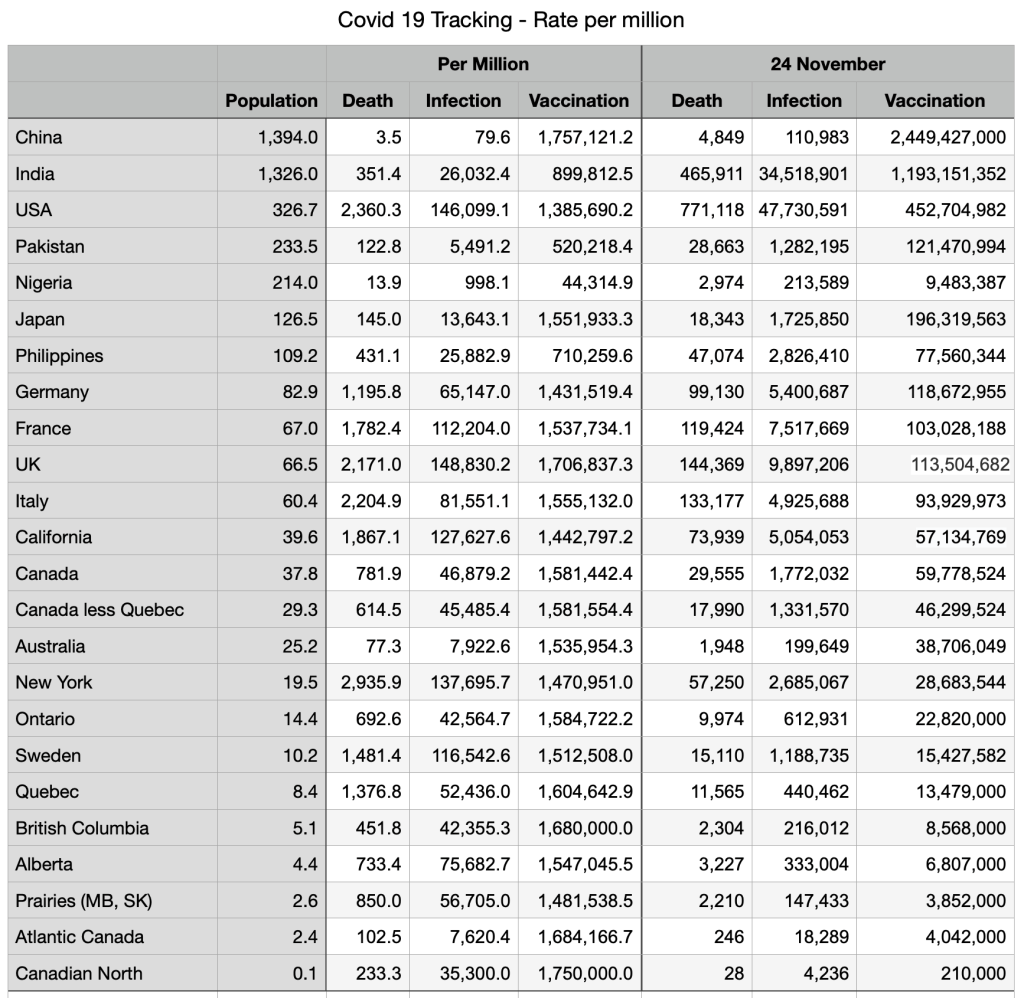
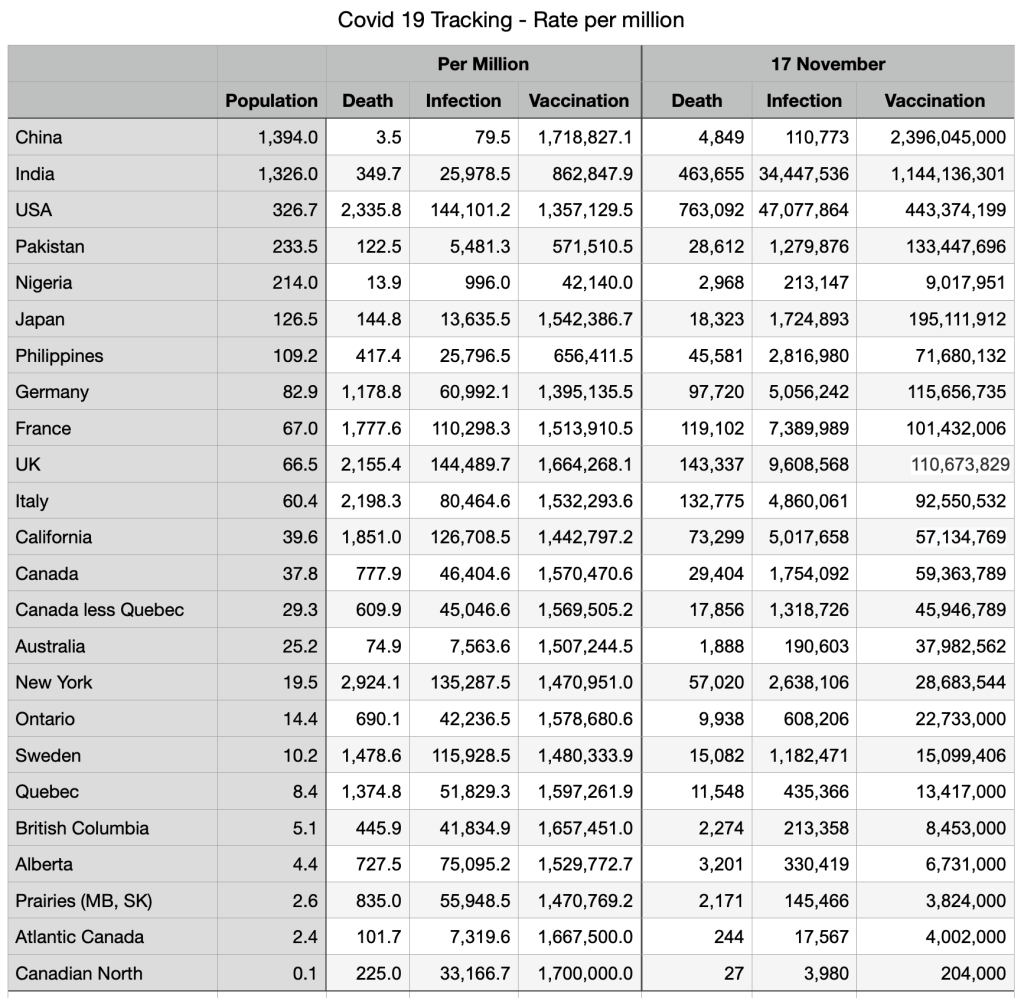
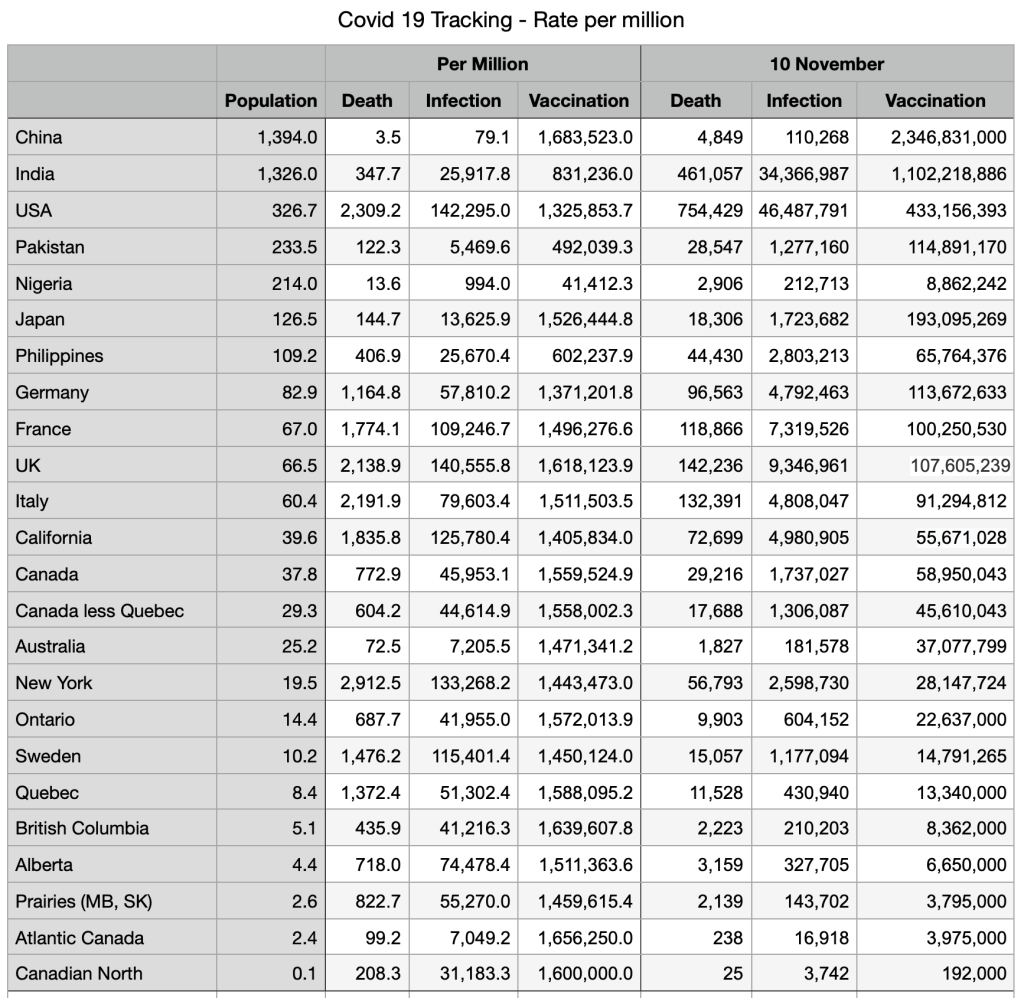
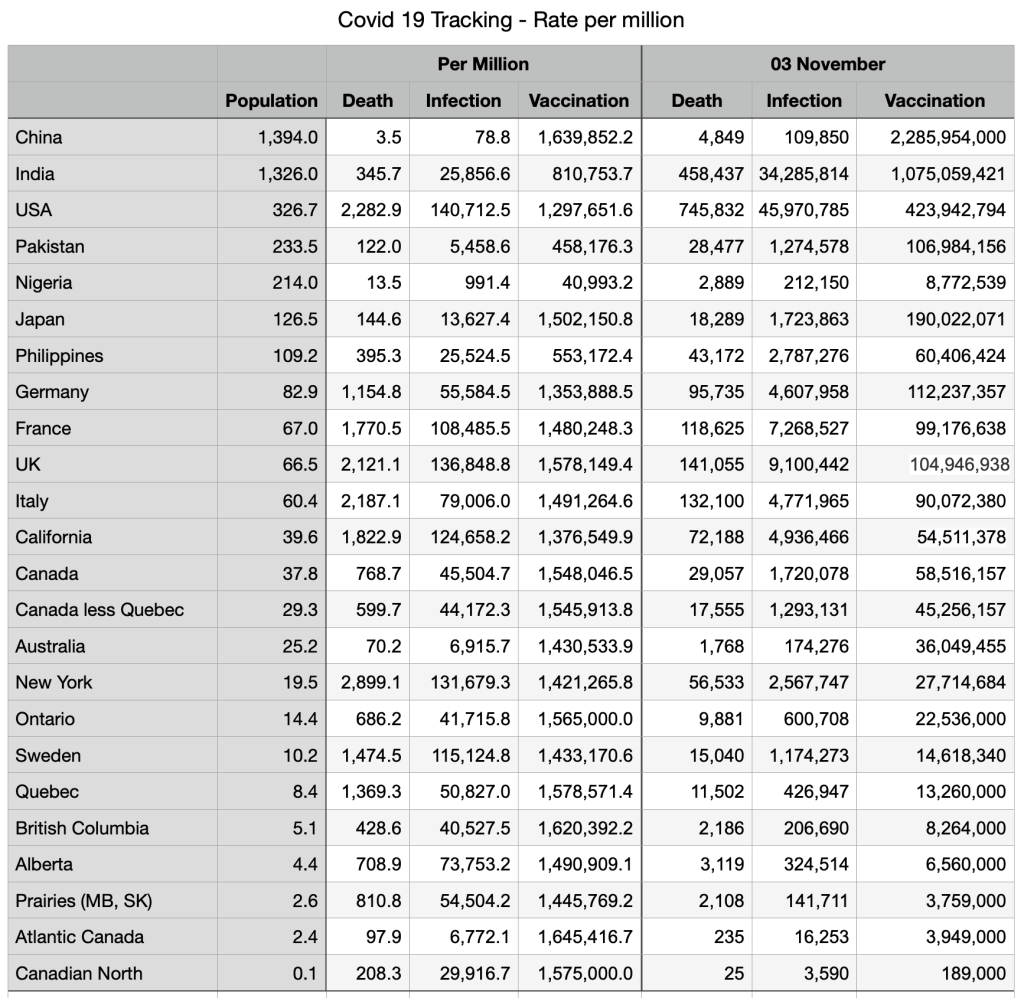
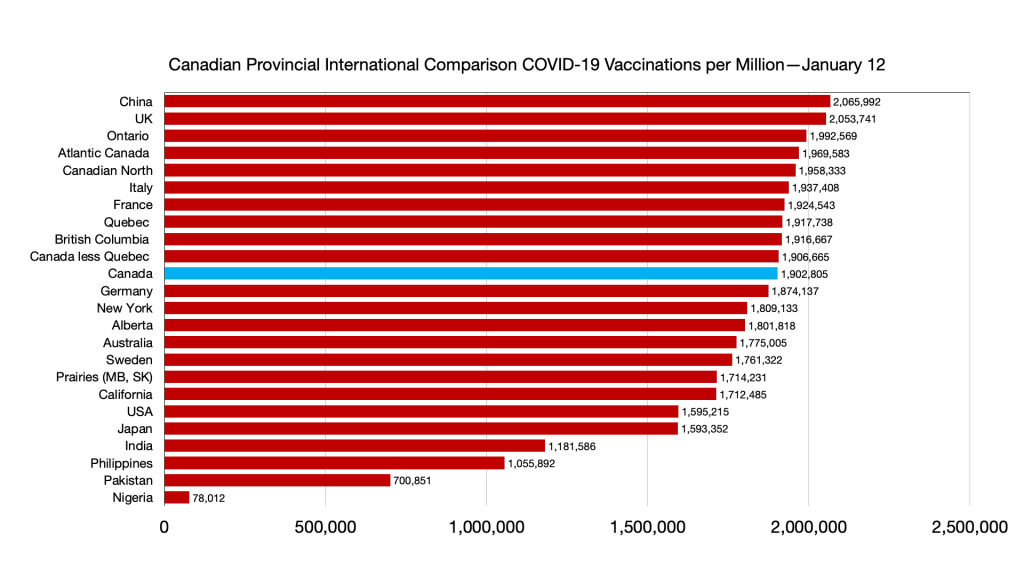
Vaccinations: Some minor shifts but general convergence among provinces and countries. Canadians fully vaccinated 78.7 percent, compared to Japan 78.8 percent, UK 71.4 percent and USA 63.4 percent.
Immigration source countries are also converging: China fully vaccinated 87 percent, India 46.8 percent, Nigeria 2.4 percent (the outlier), Pakistan 34.7 percent, Philippines 49.4 percent.
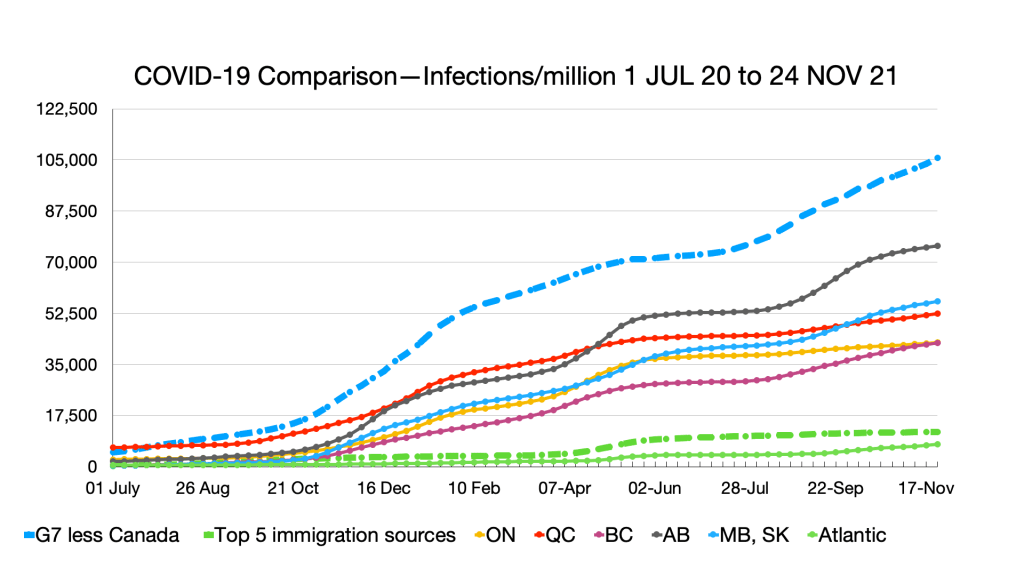
Trendline Charts:
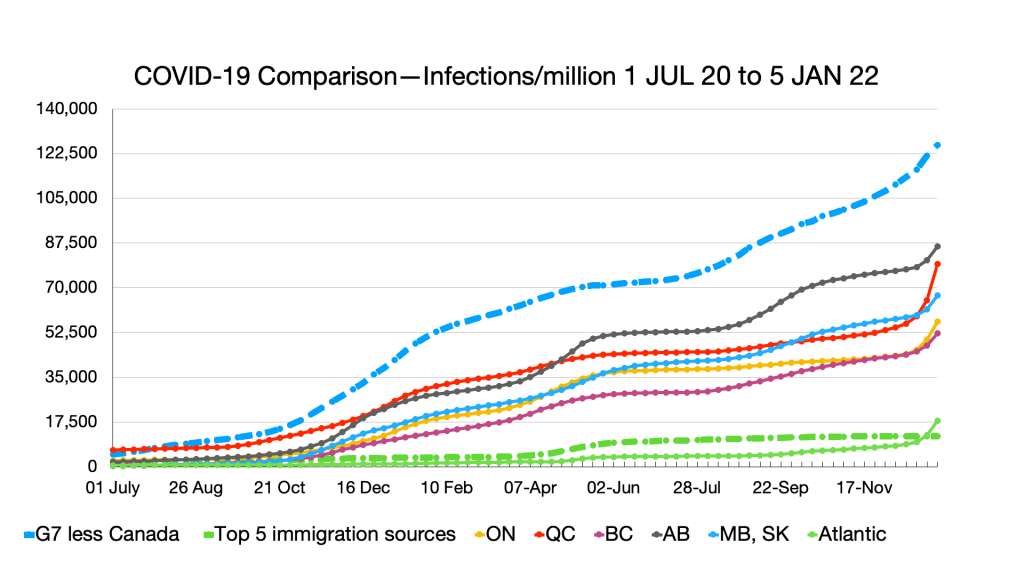
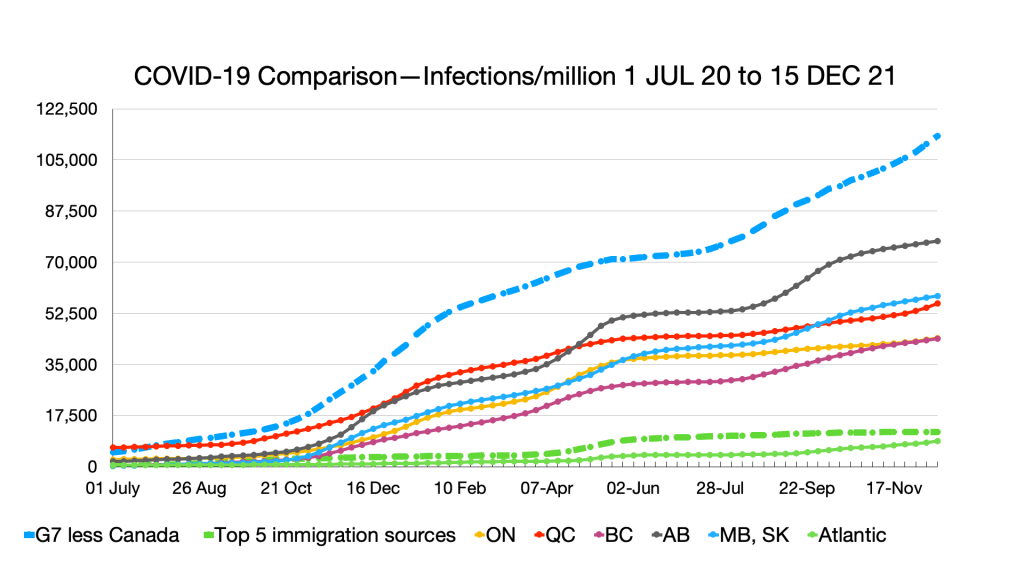
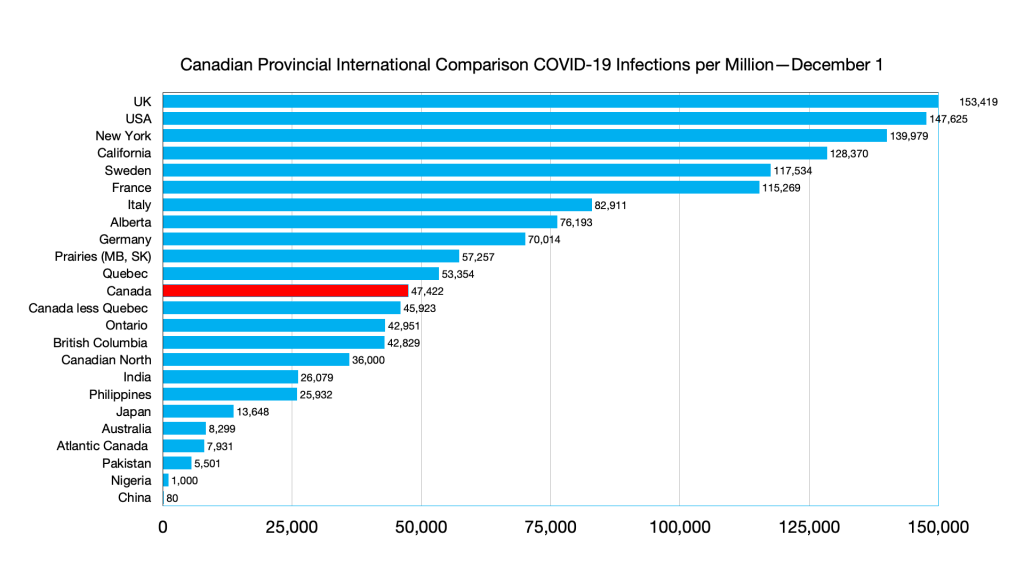
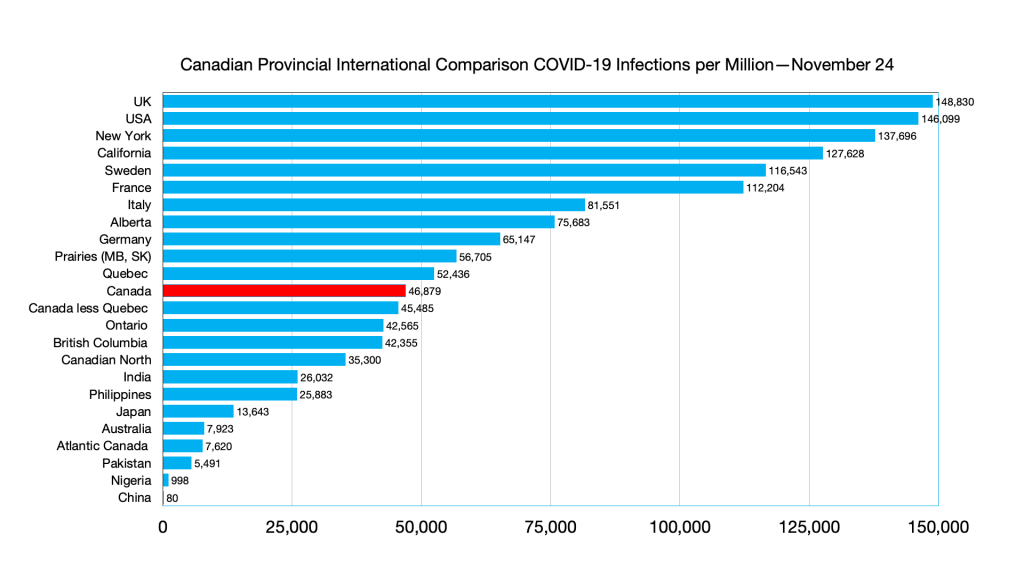
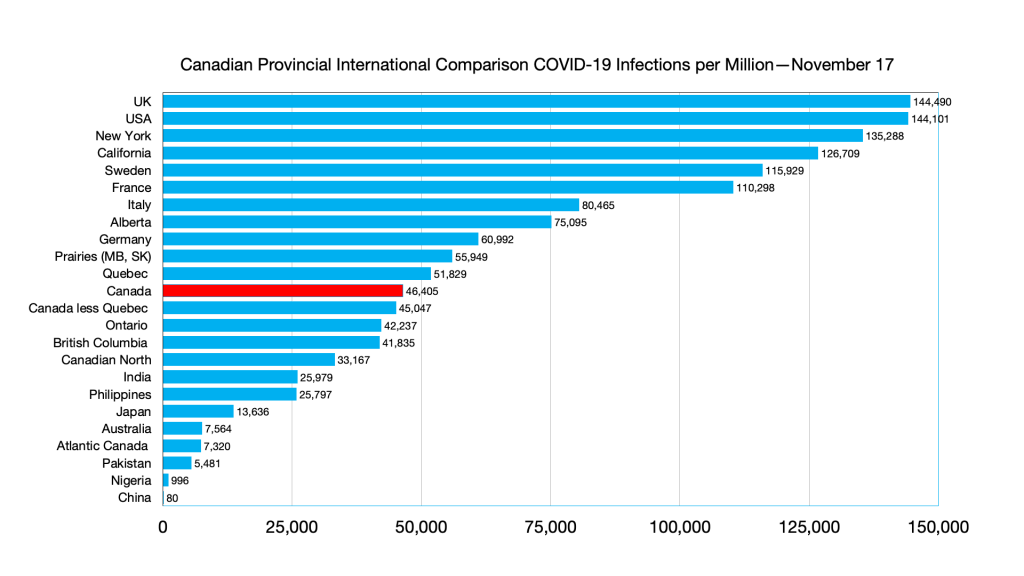
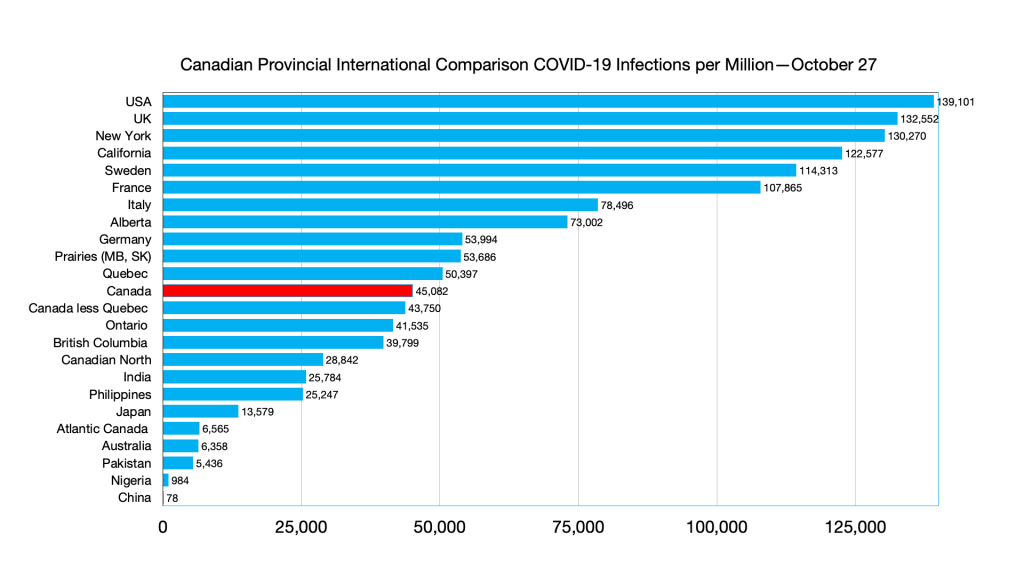
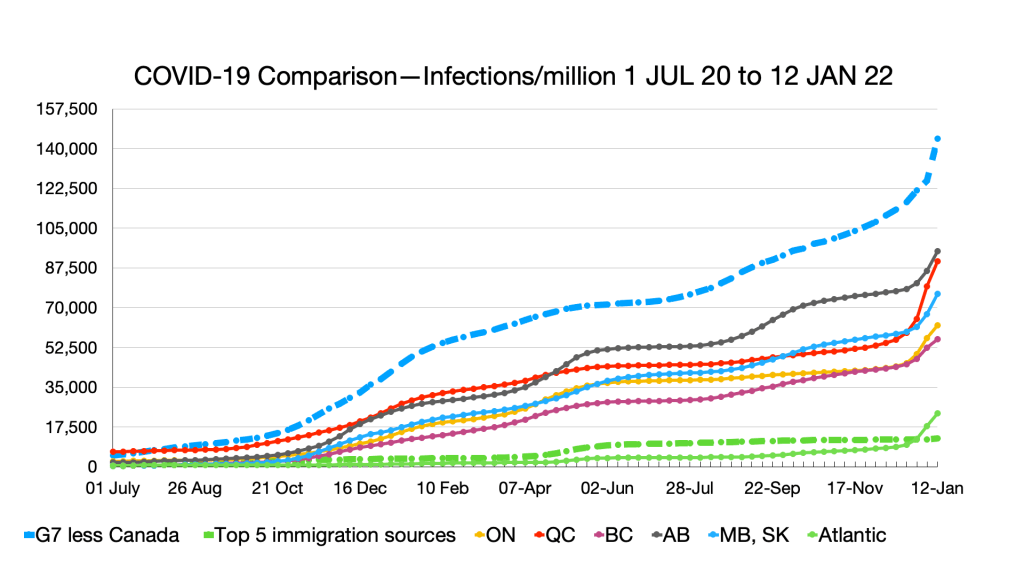
Infections: Effects of Omicron seen in steep curve in all G7 countries and provinces. No such effect in immigration source countries
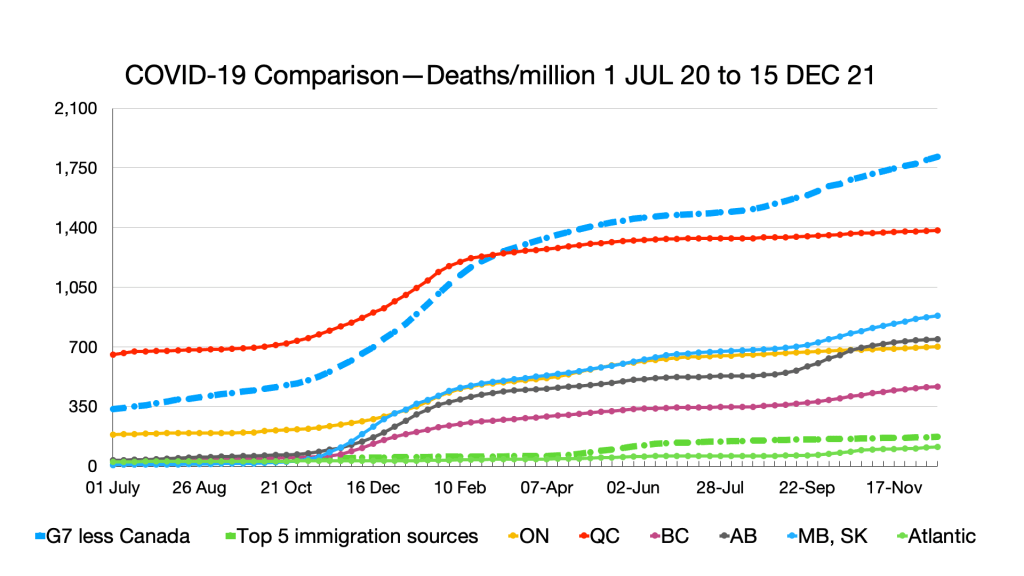
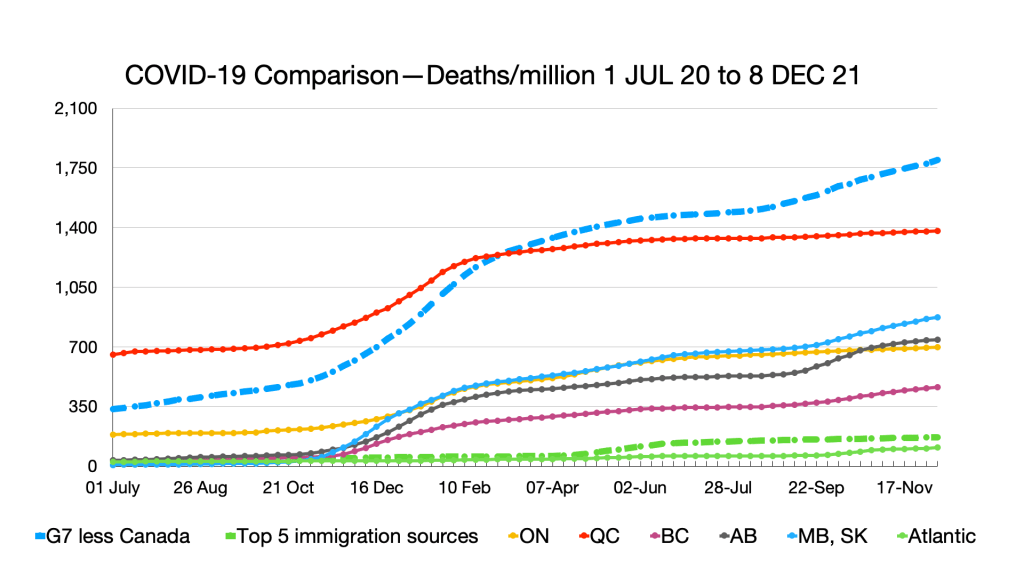
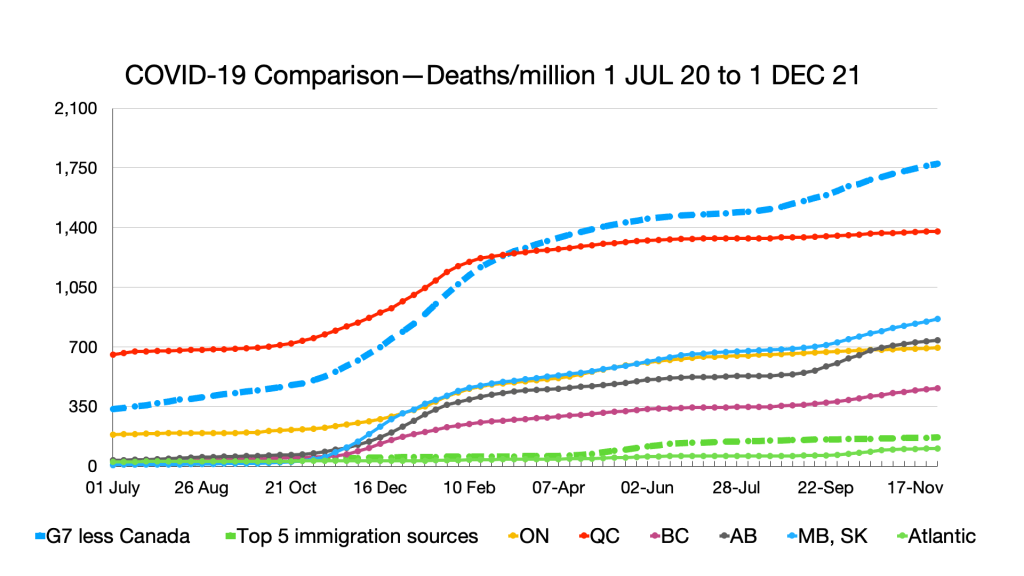
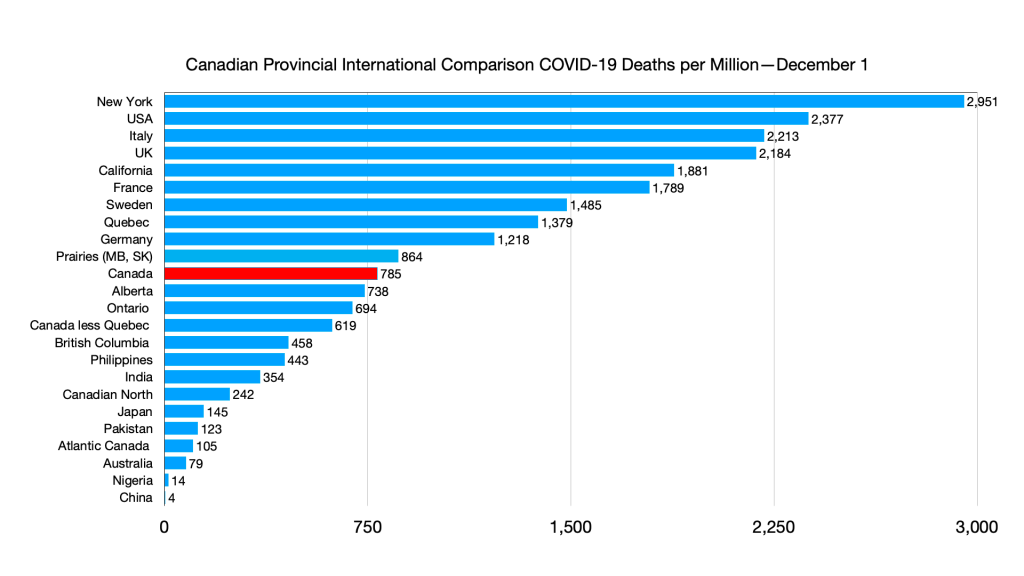
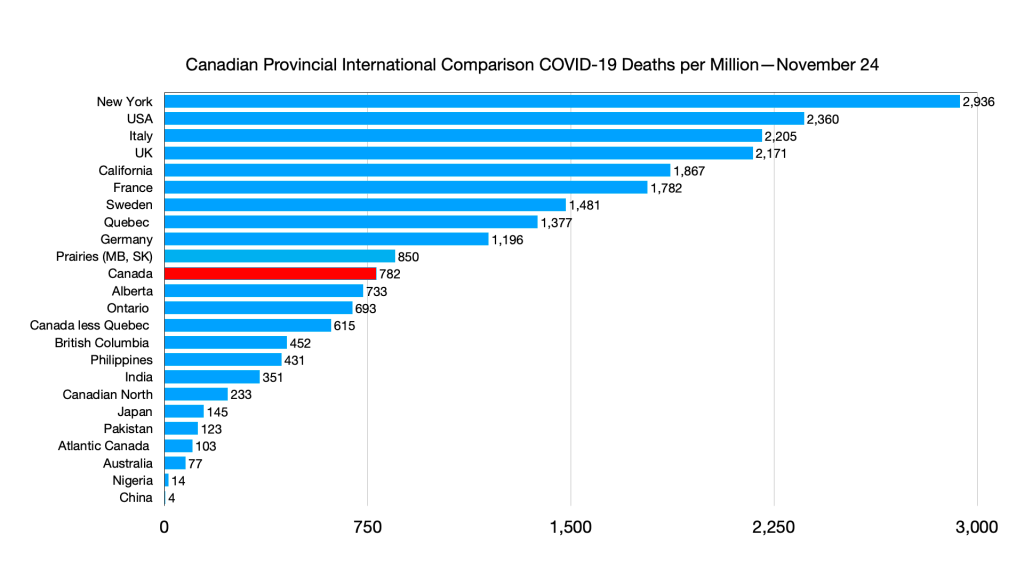
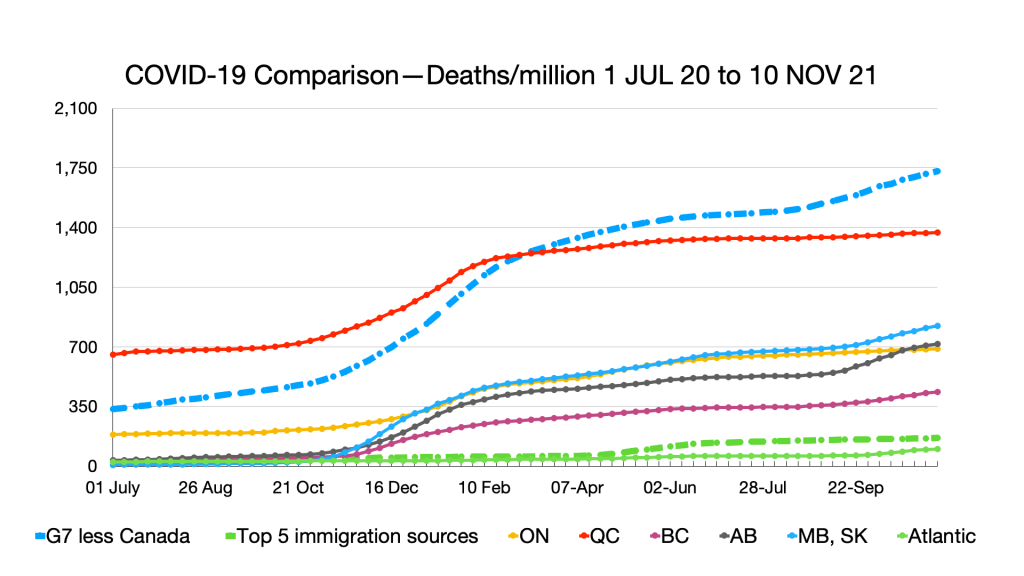
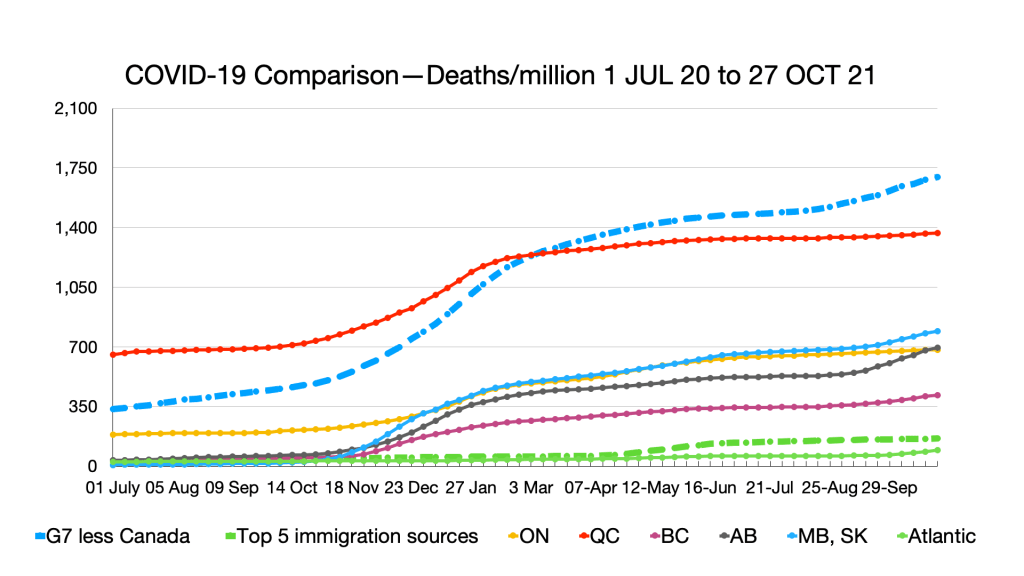
Deaths: No relative changes but slight uptick in Quebec.
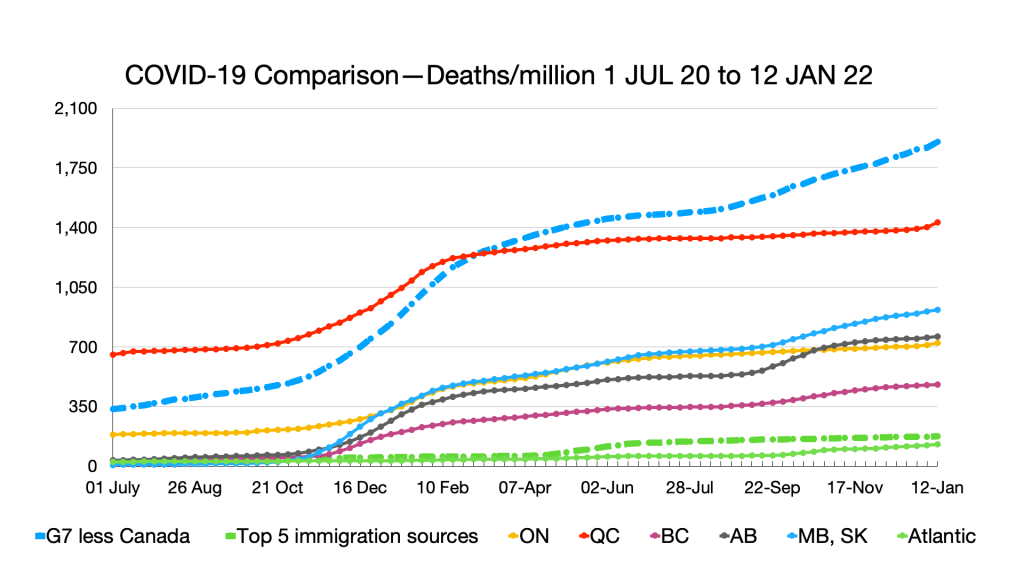
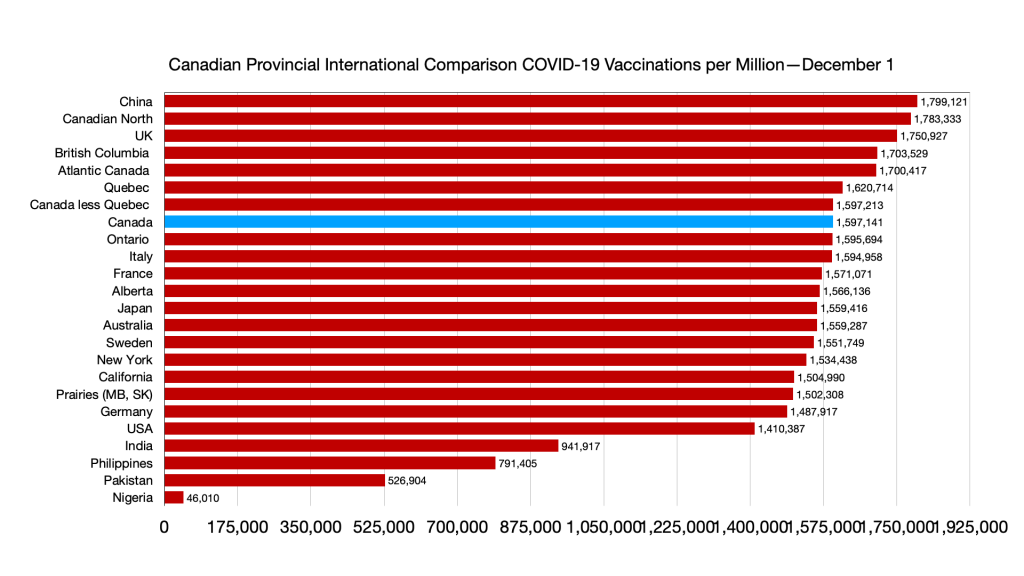
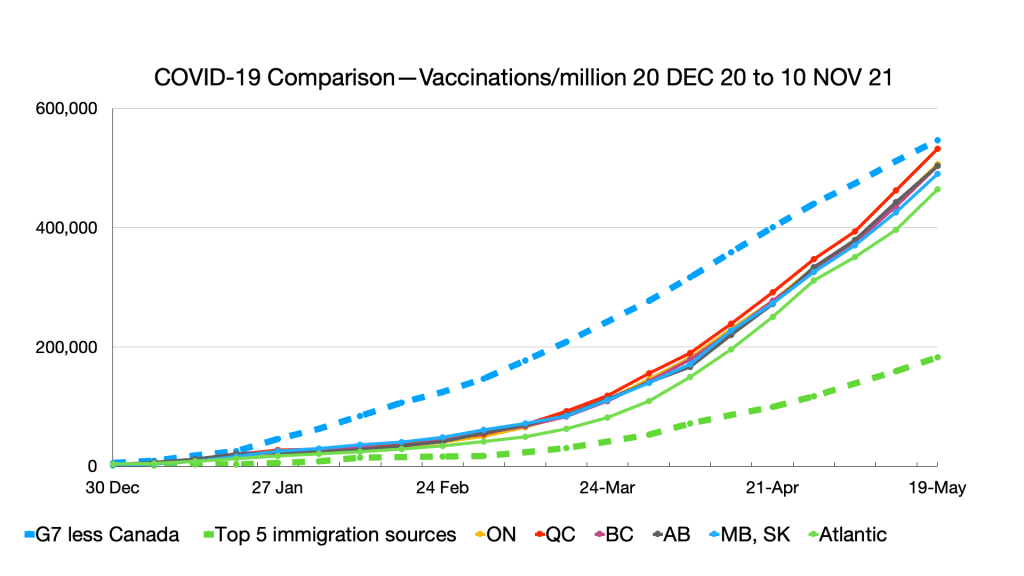
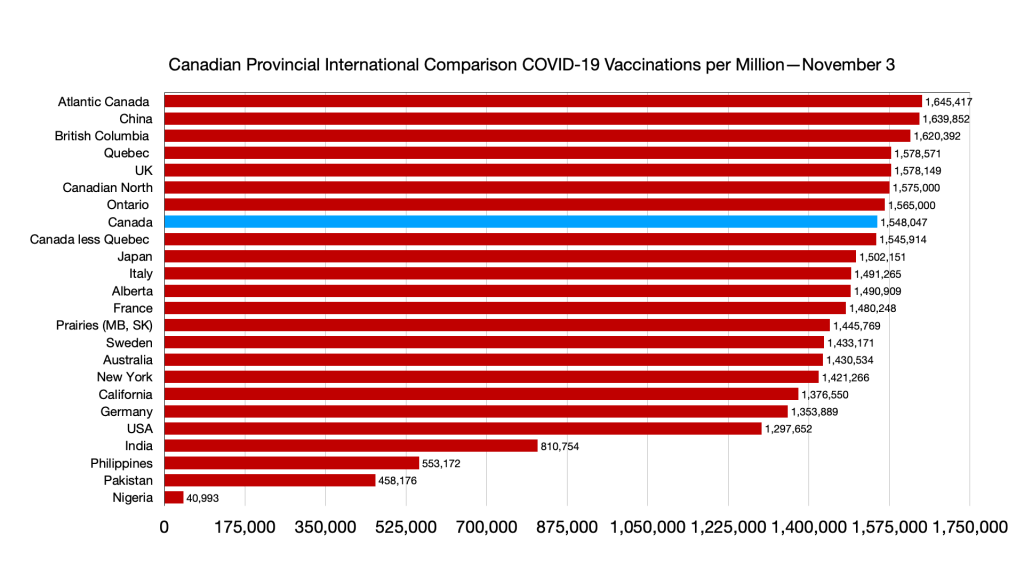
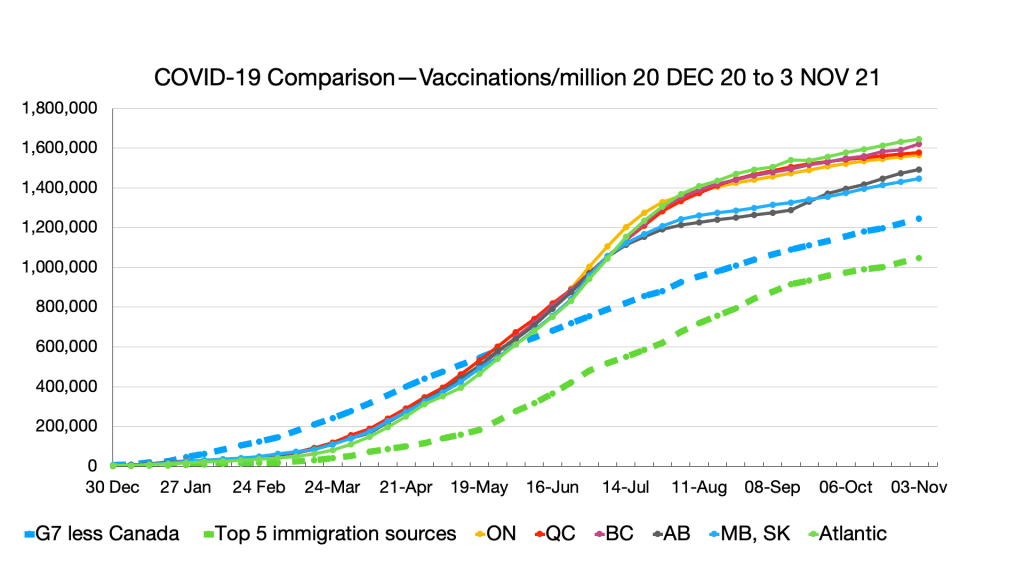
Vaccinations: Ongoing convergence among provinces and G7 less Canada and narrowing gap with immigration source countries. Nigeria remains the laggard.
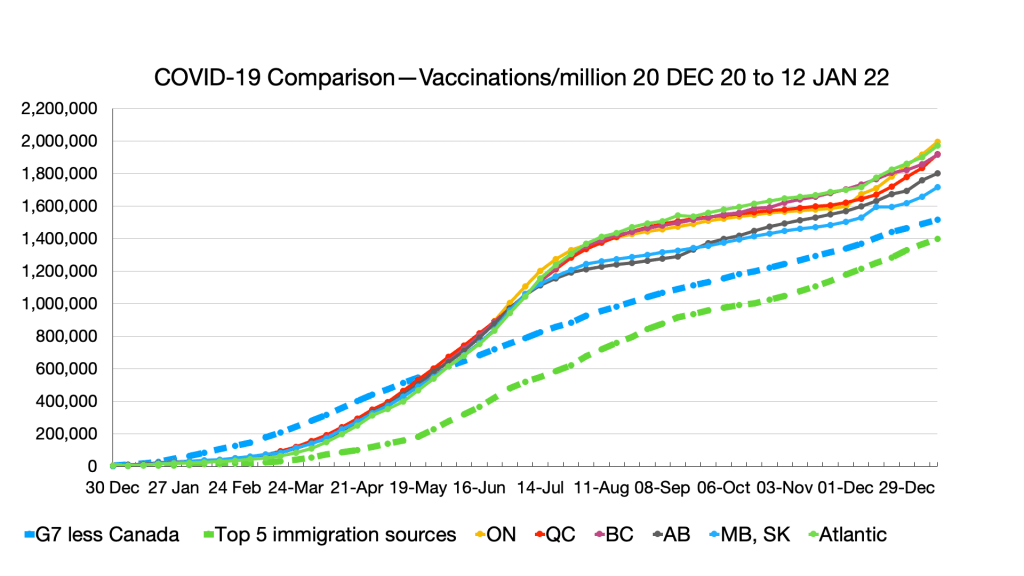
Weekly
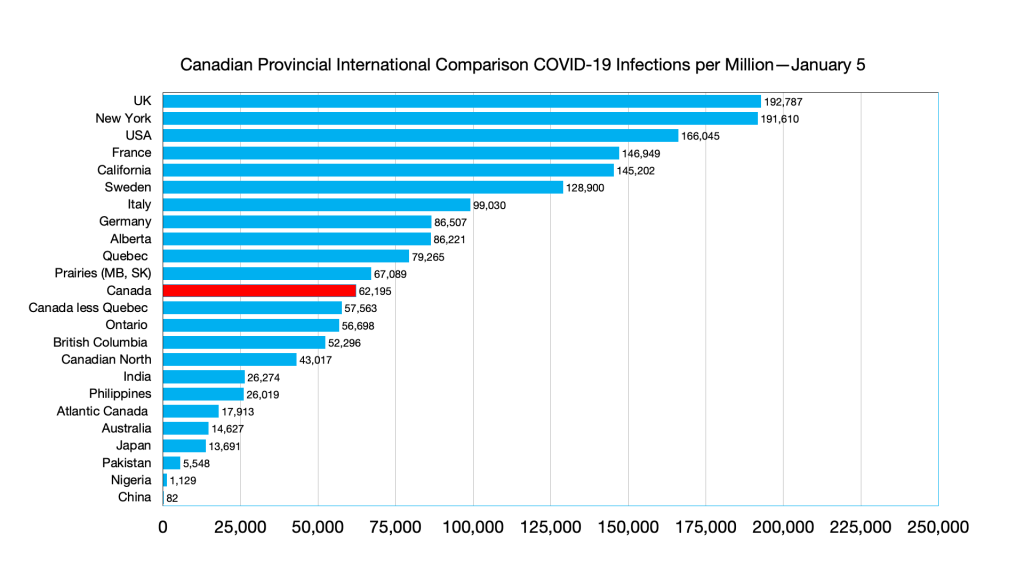
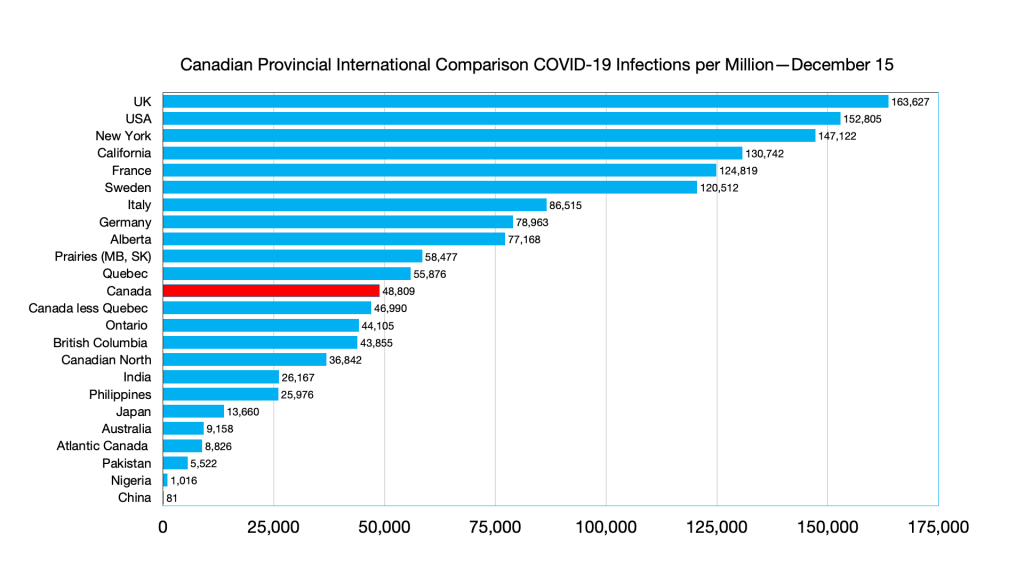
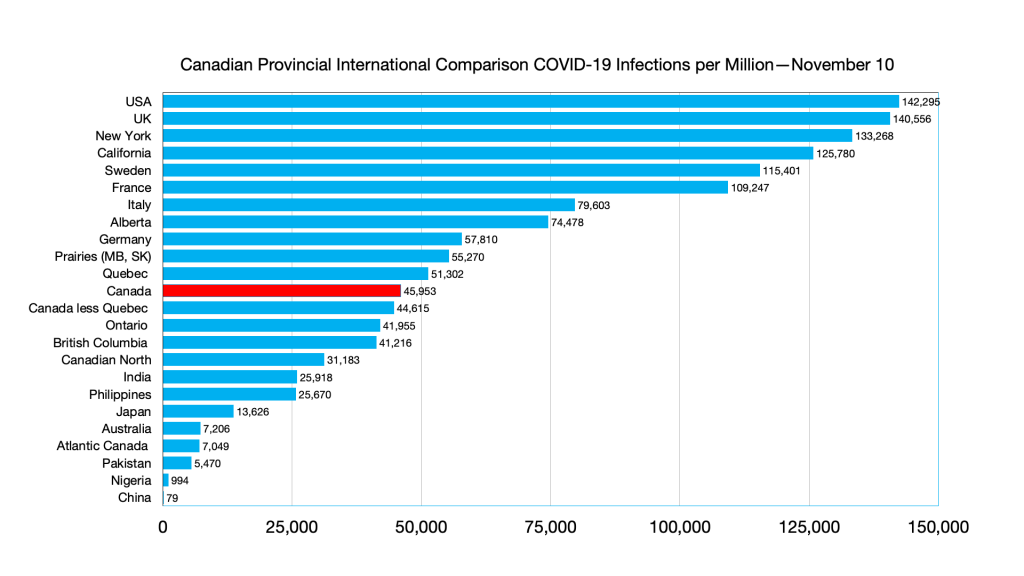
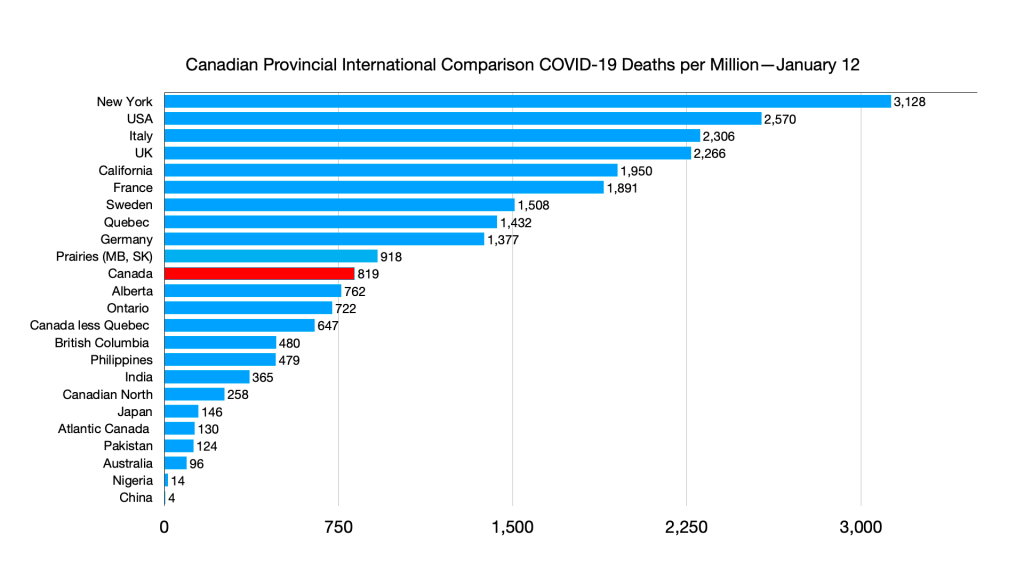
Infections: Alberta ahead of Germany, Australia and Philippines ahead of India, India ahead of Atlantic Canada.

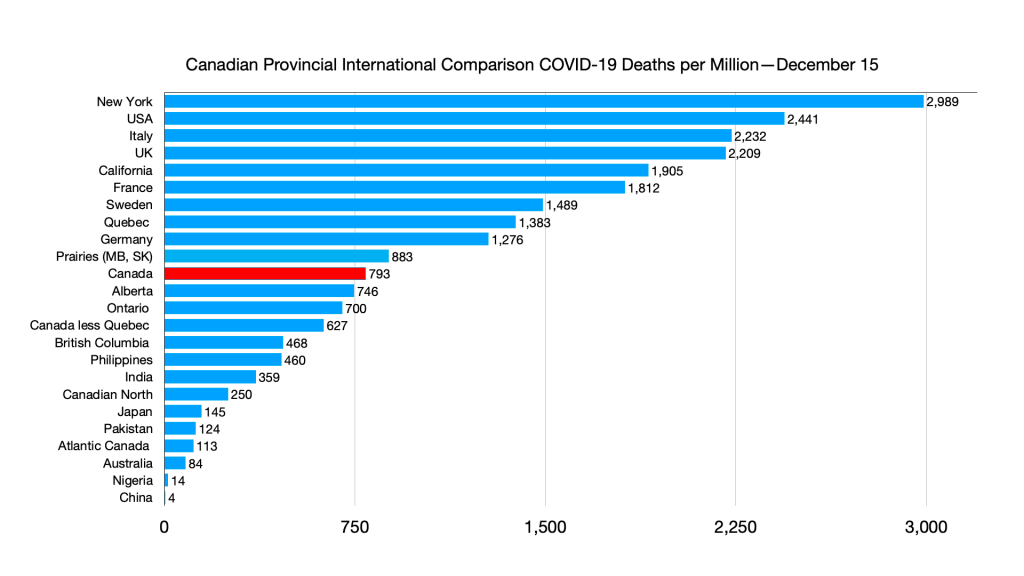
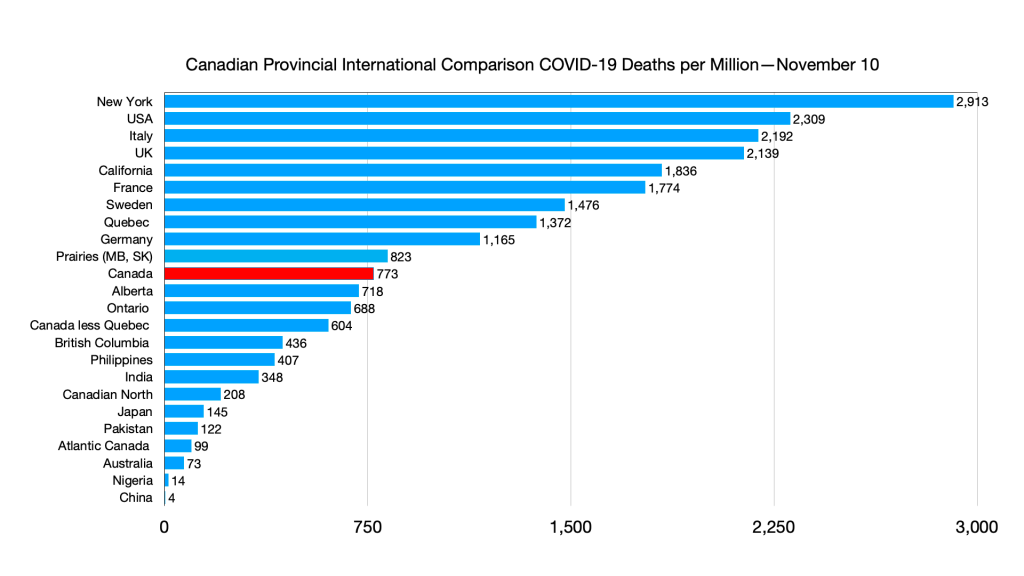
Deaths: Atlantic Canada ahead of Pakistan.

Fair amount of commentary on Quebec’s announcement of a health tax on the unvaccinated, with most commentary opposed to the idea. A notable exception on the right side of the political spectrum, Tasha Kheiriddin:
What to do about the unvaccinated? As Omicron tears through Canadian society, this public health question has become a political wedge issue. The Liberals and Conservatives have chosen sides, ramped up the rhetoric, and polarized the debate, each playing to the base they think is most likely to support their point of view.
With 88 per cent of Canadians over the age of 12 fully vaccinated , the Liberals figure they’re pretty safe siding with the crowd that favours the jab. Regrettably, they have chosen the strategy of demonization. On Friday, Health Minister Jean-Yves Duclos speculated provincial governments would make vaccination mandatory, which he said could be needed to get “rid” of the virus.
During the election campaign Prime Minister Justin Trudeau called the unvaccinated “misogynists and racists.” He dialled that down a bit last week when he said that Canadians are angry at the unvaccinated who take up hospital beds, but his remarks caused a furor that has yet to subside. This is not accidental.
The sad reality is that there is a subset of the unvaccinated who fit Trudeau’s description; since September, for example, some have been using the hashtag “Pureblood” on social media to self-identify as unvaccinated. You don’t have to scroll far to find tagged images peppered with shots of white supremacy gestures or MAGA hats.
The Liberals’ dogwhistle is designed to conflate these people with mainstream Conservatives — and turn people off Conservative Leader Erin O’Toole’s call for “reasonable accommodation.” O’Toole is asking for “acceptance” of the fact that up to 15 per cent of the population will not get vaccinated. He favours using rapid tests to keep unvaccinated workers on the job, as opposed to shutting down to stop the spread of the virus.
“In a population that is now largely fully vaccinated, in fact the action and inaction by the Trudeau government is normalizing lockdowns and restrictions as the primary tool to fight the latest COVID-19 variant.”
But this approach is also wrong. First, it relies on unreliable technology. Rapid tests are not good at detecting Omicron infections, particularly in the early stage when a person is infectious but shows no symptoms. Second, it sends a double message. On the one hand, the Tories encourage people to “get vaccinated.” On the other, they make allowances for those who eschew the jab. It’s like saying “wear your seatbelt, but if you don’t, that’s OK.” Well guess what — it’s not. If you get in an accident, it will cost up to three times more to treat you in hospital than if you were buckled up. Sound familiar?
The reality is that we restrict plenty of behaviours where we judge the harm to others, including economic harm, outweighs the limits to individual liberty. We don’t allow people to smoke in workplaces or public buildings. We forbid drinking and driving. And we mandate vaccination for contagious diseases such as measles if children are to attend public school. Why? Because otherwise your actions, or inaction, present a real risk of harm to someone else. They can cause quantifiable loss, in the form of sickness, suffering, even death (yes, last year 200,000 people worldwide died of measles , mostly children under five). People don’t live in a vacuum.
A liberal would cite Jean-Jacques Rousseau’s Social Contract, which called for government by popular consent; a conservative would point to Edmund Burke, who rightly observed, “Men are never in a state of total independence of each other.” In other words, there is no freedom without responsibility, no liberty without duty.
When it comes to vaccination, we should protect those who understand this truth from those who disdain it. Vaccine passports, restrictions on interaction and withdrawal of privileges are preferable to calling people names, forcing them to get the shot, or conversely accommodating a choice that puts others in harm’s way. Obliging those who opt out of vaccination to pay a penalty, such as the Quebec government is suggesting, is also a possibility. Such measures are not about cajoling or compelling, though if they do result in more vaccinations, that’s a good thing. They are meant to protect all of us who just want to move on from this once-in-a-century public emergency and get back to living our lives
Source: The unvaccinated must be deterred from harming others