My assessment:
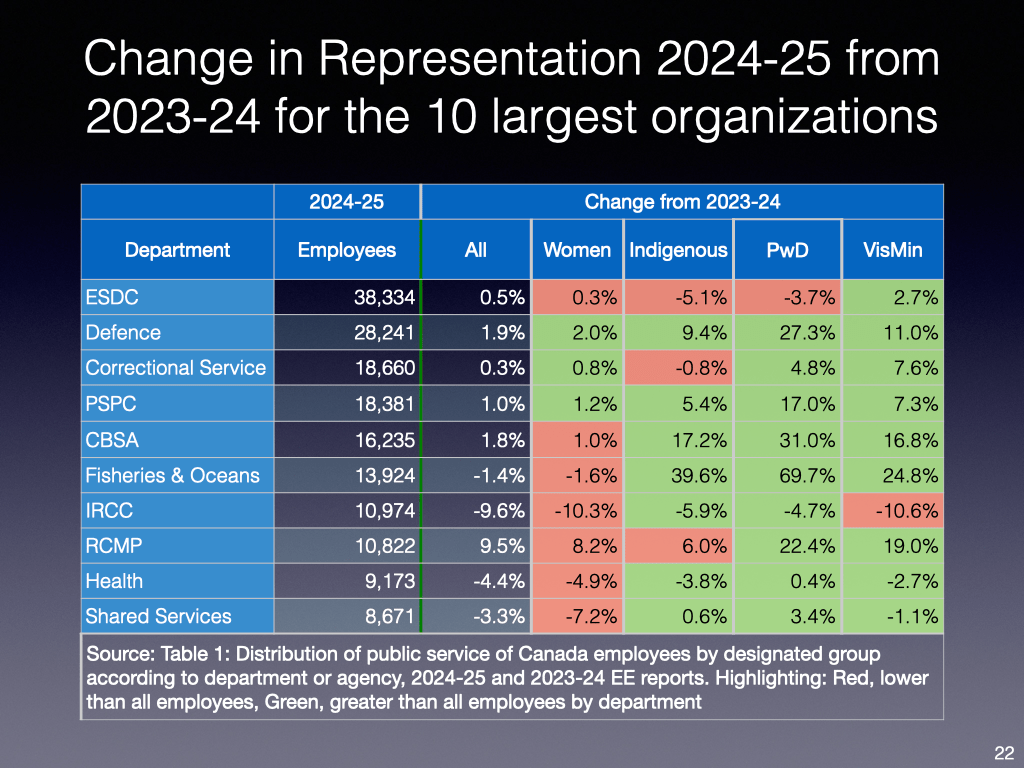
The most recent report on diversity in the public service says hiring dipped by 40 per cent last year as the bureaucracy began reversing course on a decade of significant growth. But this appears to have had limited impact on equity efforts.
New data on employment equity in the federal public service shows initial attempts to shrink the population had a limited effect on the proportions of equity-seeking groups. But one expert on public policy and governance says coming job cuts are “agnostic” to these efforts, and a large public-sector union says the government isn’t doing enough to ensure diversity is maintained amid sweeping job cuts.
“I can’t see evidence that minority groups are being penalized compared to majority groups,” said Andrew Griffith, a former public servant who was a director general of citizenship and multiculturalism at then-Citizenship and Immigration Canada….
Griffith noted concerns about job cuts in the public service hampering progress in employment equity, but so far that doesn’t seem to be the case.
“Now, it might change in the current year, given the cutbacks are more significant this year,” said Griffith, referring to the approximately 24,000 public servants who have already received notice that their jobs might be at risk, and the some 9,000 jobs expected to be cut….
“The numbers don’t tell the whole story”: Turnbull
Lori Turnbull is a political science professor at Dalhousie University, a senior adviser at the Institute on Governance, and worked in the Privy Council Office from 2015 until 2017.
Speaking to The Hill Times, she said the high percentage of women “really makes it look like the public service is doing well,” in terms of equity among its ranks, but “that doesn’t really speak to what’s going on for other groups,” she said.
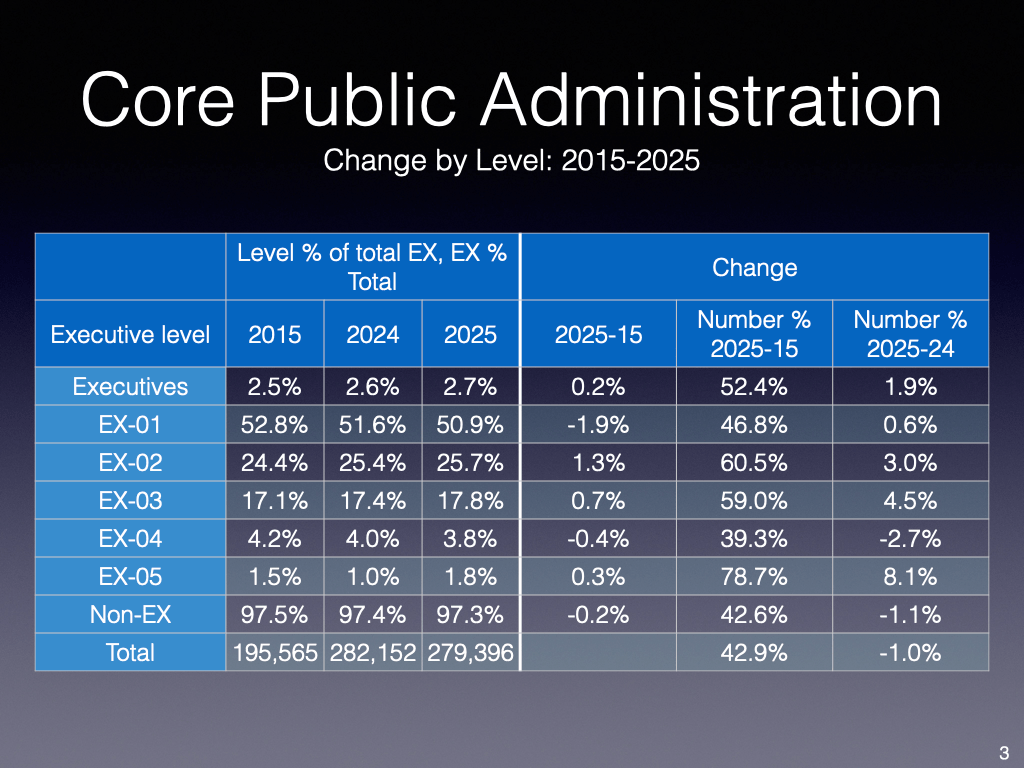
“I don’t think anybody would come away from that and think, ‘Oh, we better be worried because the share of women [being hired] decreased by three points,” Turnbull said, noting the high number of women in executive positions as well as the broader public service.
However, she noted the current spending review that is expected to shed thousands of jobs from the public service is “agnostic” to employment equity considerations.
“It just doesn’t really sound like there’s much co-ordination in that,” she said.
“The way they’re measuring [it] is by the numbers, by the money, and not by the function and the specific people,” she said.
“You get the numbers, and it doesn’t tell the whole story.”
Sean O’Reilly, president of the Professional Institute of the Public Service of Canada, one of the largest federal public service unions, said the government isn’t doing enough to protect equity-seeking groups from cuts.
“There are big concerns,” he said. “Some of the correlation we’ve seen in the past with cuts, and we fear that, we do fear that these groups will be unjustly affected by all these cuts.”
Source: Treasury Board report shows employment equity not affected by early phases of public service job losses in 2024-25 Paywall