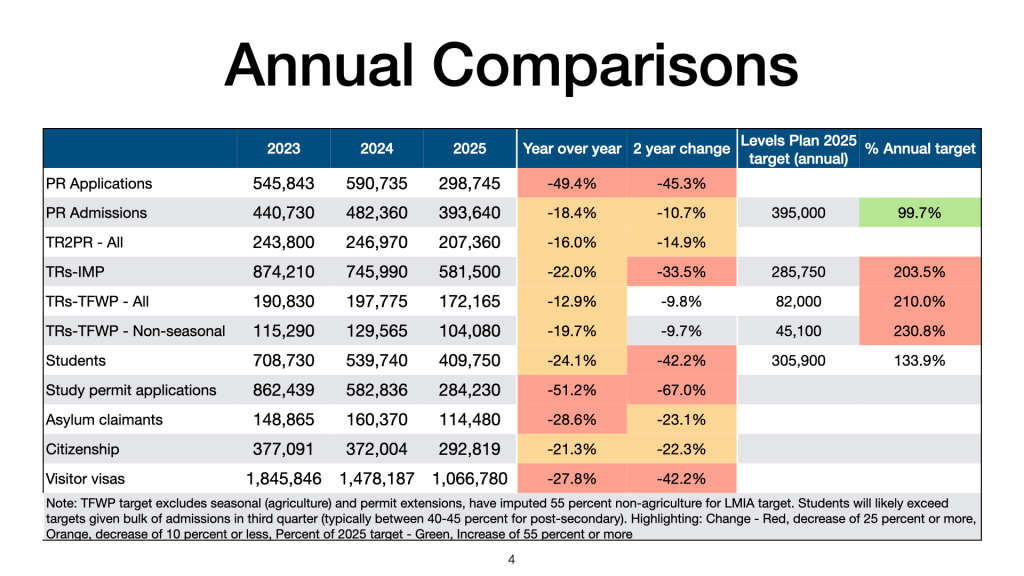
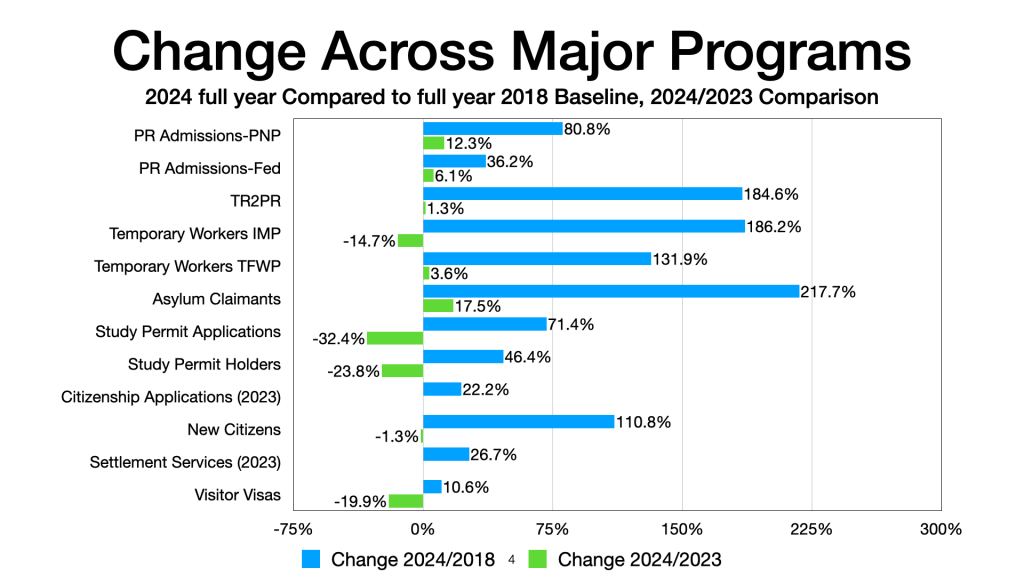My regular update on key immigration programs. Given the various articles on whether or not the government is meeting the reductions announced earlier, here is where we stand for January to June for the current and previous two years:
Permanent residents admissions: From 255,015 in 2024 to 207,510 in 2025, decline 18.6 percent, (from 2023, decline 21 percent), about 50 percent of 2025 target
TR2PR (Those already in Canada): From 148,020 in 2024 to 126,365 in 2025, decline of 14.6 percent (from 2023, decline 13 percent).
TRs-IMP: From 420,070 in 2024 to 295,505 in 2025, decline of 29.7 percent (from 2023, decline 23.4 percent), already exceeds 2025 target
TRs-TFWP: From 110,910 in 2024 to 106,105 in 2025, decline of 4.3 percent (from 2023, decline 7.2 percent), already exceeds 2025 target for both agriculture and non-agriculture workers
Students: From 248,820 in 2024 to 152,775 in 2025, decline of 38.6 percent (from 2023, increase 26.1 percent), about 50 percent of 2025 target (likely to overshoot given third quarter has highest number of admissions (between 40-45 percent for post-secondary albeit only 34 percent in 2024)
Asylum Claimants: From 93,315 in 2024 to 57,810 in 2025, decline of 38 percent (from 2023, decline 3.7 percent)
Citizenship: From 205,363 in 2024 to 151,804 in 2025, decline of 26.1 percent (from 2023, decline 14.2 percent)
Visitor Visas: From 868,234 in 2024 to 568,195, decline of 34.6 percent (from 2023, decline 40.5 percent)